According to an analysis undertaken by experts from UCL and the Royal Devon and Exeter Hospital, a change in clinical practice would have clear benefits for patients undergoing major bowel surgery.
The study, published in The British Journal of Surgery, shows that administering iron intravenously before colorectal surgery improves patient outcomes by 33 per cent, lowering the need for blood transfusions.
Anaemia is a common issue in individuals undergoing colon surgery due to gastrointestinal bleeding and blood loss during the procedure. Anaemia is also linked to fatigue and illness following surgery, as well as a longer recovery and other consequences.
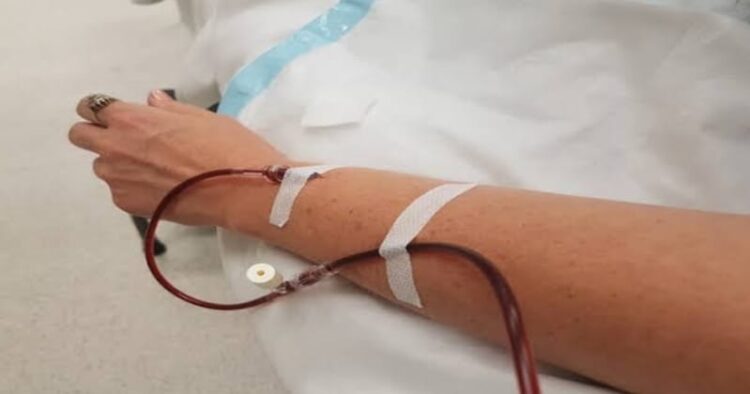
Blood transfusion is utilised when blood levels are low, but there is worry that colorectal cancer patients who have had a blood transfusion may have a higher likelihood of problems and cancer recurrence. Anaemia is frequently treated with iron, with a full course of medication administered intravenously in 15-30 minutes. To yet, intravenous iron infusion has been utilised rarely, with the question of whether treating patients before major surgery will lessen the need for blood transfusions remaining unanswered.
Researchers from UCL conducted a meta-analysis of five randomised controlled trials in this study, concentrating on a subset of patients from those trials who had undergone colon surgery.
The analysis showed that patients who had received iron infusion were 33 per cent less likely to require a blood transfusion during or after surgery.
Patients were divided into two groups in these trials: a control group and a group that got iron intravenously prior to surgery.
Professor Toby Richards, senior author of the study from UCL Division of Surgery & Interventional Sciences, said, “This is the first time that clinical trials have shown a patient benefit from treatment with an iron infusion before surgery, which has the potential to treat anaemia and reduce the need for blood transfusion. Previous studies had not shown this benefit for all patients undergoing surgery in the NHS, but this analysis identifies a subset of patients undergoing bowel surgery who will see a benefit.”
Professor Neil Smart, colorectal surgeon from the Royal Devon and Exeter Hospital and co-lead of the study, said, “With over 20,000 major colorectal cancer resections per year in the UK, the findings of this study have the potential to improve outcomes for the second most common cause of cancer mortality. In the past, surgeons were uncertain whether the benefits of iron infusion could be realised in the short time frames of cancer care and consequently the uptake of this treatment was limited. Our findings show that improved outcomes can be achieved if iron infusion is given in the period between cancer diagnosis and surgery.”
As well as reducing the risk for patients, fewer blood transfusions would be good news at a time when there are blood supply shortages in the UK.
Sue Pavord, Vice President of the British Society for Haematology, said, “The recent shortage of blood supply in the UK means it is more important than ever to focus on ways to avoid blood transfusions and their associated risks. This analysis shows a reduction of over one-third in blood transfusions when anaemic patients are treated with intravenous iron before their colorectal surgery. If we could combine this insight with others from the previous PREVENT study, then hospital readmissions could potentially be cut even more, which would be important for both patients and the NHS.”
(with inputs from ANI)